Conjunctivitis (Pink Eye)
Inflammation of the clear membrane covering the eye and inner eyelids. Learn about viral, bacterial, and allergic types, symptoms, and treatment.
Conjunctivitis, commonly called "pink eye," is inflammation of the conjunctiva—the clear membrane covering the white of the eye and lining the inner eyelids. It's one of the most common eye conditions and has several different causes, each requiring different management.
Key Takeaways
- Three main types: viral (most common), bacterial, and allergic
- Viral conjunctivitis is highly contagious and usually resolves on its own in 1-2 weeks
- Bacterial conjunctivitis produces thick discharge and may need antibiotic drops
- Allergic conjunctivitis causes itching and is not contagious
- Good hygiene is essential to prevent spread of infectious types
- Specialized types (gonococcal, chlamydial, neonatal) are less common but may require urgent treatment
What Are the Different Types of Conjunctivitis?
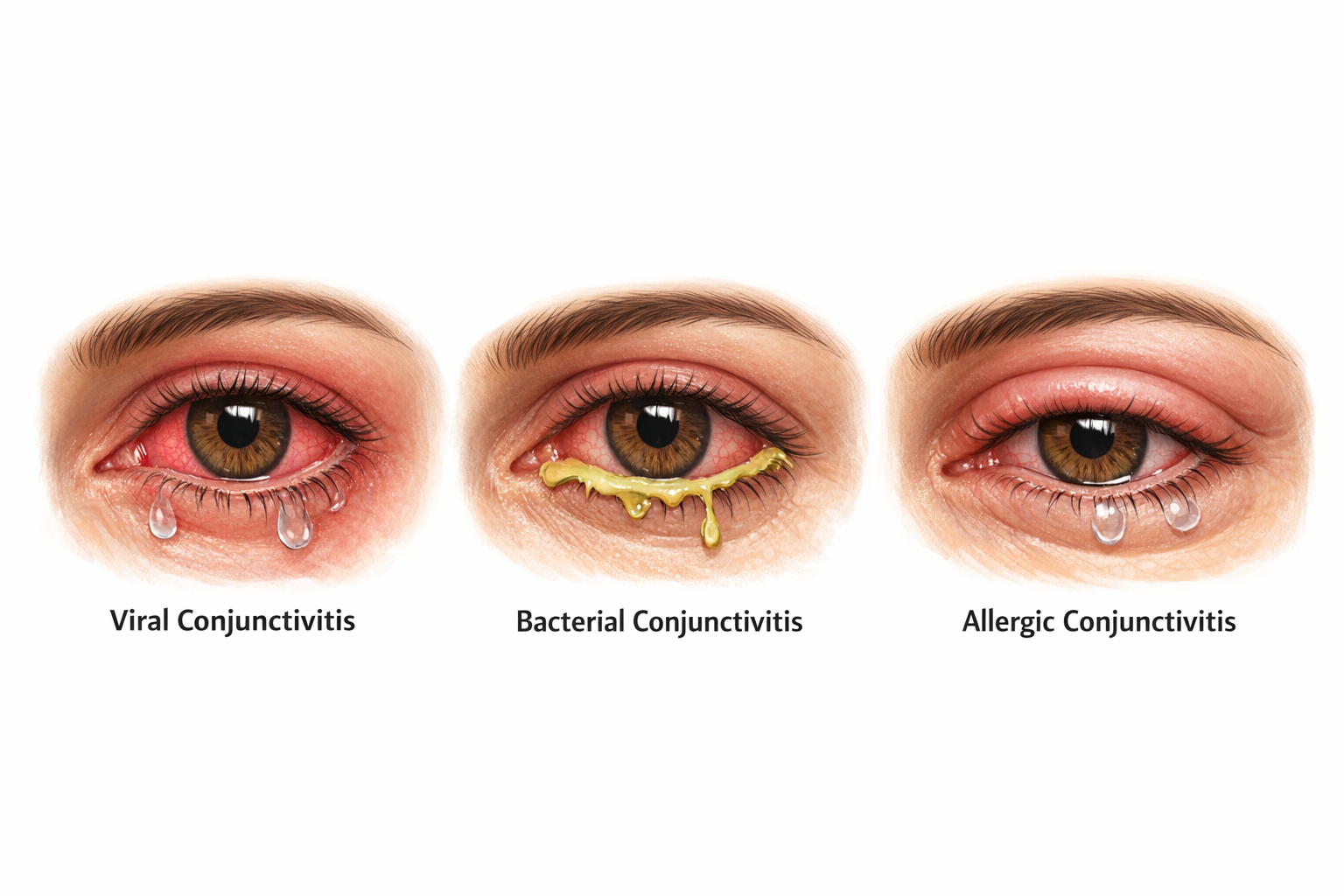
There are seven main types of conjunctivitis, each with different causes, symptoms, and treatments. The three most common are viral, bacterial, and allergic. The type determines whether the condition is contagious and what treatment is needed. For a patient-friendly comparison of the three main types, see our guide on bacterial vs viral vs allergic pink eye.
At a Glance: Conjunctivitis Types Compared
| Type | Key Symptoms | Cause | Contagious? | Typical Treatment | Duration |
|---|---|---|---|---|---|
| Viral | Watery discharge, redness, cold symptoms | Adenovirus, other viruses | Yes — highly | Supportive care (cold compresses, artificial tears) | 1–3 weeks |
| Bacterial | Thick yellow-green discharge, crusting | Staph, Strep, Haemophilus | Yes | Antibiotic eye drops | 5–7 days with treatment |
| Allergic | Intense itching, watery eyes, puffiness | Pollen, dust, pet dander | No | Antihistamine drops, allergen avoidance | While exposed to allergen |
| GPC | Itching, mucus, lens intolerance | Contact lens wear | No | Lens modification, anti-inflammatory drops | Weeks to months |
| Gonococcal | Copious pus, severe swelling | N. gonorrhoeae (STI) | Yes | Emergency systemic antibiotics | Days with urgent treatment |
| Chlamydial | Chronic redness, mild discharge | C. trachomatis (STI) | Yes | Oral antibiotics | Weeks |
| Neonatal | Discharge in newborn (first 28 days) | Various (depends on timing) | Varies | Depends on cause — may be emergency | Varies |
Viral Conjunctivitis
Most common type:
- Highly contagious; often starts in one eye and spreads to the other
- Watery discharge, frequently linked to a recent cold
- Resolves on its own in 1–2 weeks without antibiotics
- In rare cases, influenza viruses including H5N1 (bird flu) can cause conjunctivitis — see our guide on pink eye and bird flu
Learn more about viral conjunctivitis.
Bacterial Conjunctivitis
- Thick, yellow-green discharge that often "glues" eyelids shut overnight
- Moderately contagious
- May respond faster with antibiotic drops, though mild cases can self-resolve
Learn more about bacterial conjunctivitis.
Allergic Conjunctivitis
- Not contagious—triggered by allergens such as pollen, dust, or pet dander
- Intense itching is the hallmark symptom
- Usually affects both eyes and often accompanies sneezing or congestion
Not sure if your symptoms are from allergies or an infection? See our guide on pink eye vs allergies. Learn more about allergic conjunctivitis.
Giant Papillary Conjunctivitis
- Most commonly triggered by contact lens wear
- Characterized by large bumps (papillae) under the upper eyelid
- Treatment centers on changing or discontinuing lens use
Learn more about giant papillary conjunctivitis.
Gonococcal Conjunctivitis
- Considered an ocular emergency—can threaten vision within 24–48 hours
- Causes severe, purulent discharge
- Requires systemic antibiotics and urgent ophthalmologic care
Learn more about gonococcal conjunctivitis.
Chlamydial Conjunctivitis
- Chronic, often mild redness that may persist for weeks if untreated
- Requires oral antibiotics (topical treatment alone is insufficient)
- Sexual partners need concurrent treatment to prevent reinfection
Learn more about chlamydial conjunctivitis.
Neonatal Conjunctivitis
- Occurs in newborns within the first month of life; timing of onset helps guide diagnosis
- Erythromycin ointment is given at birth as prophylaxis
- Any eye discharge in a newborn warrants urgent evaluation
Learn more about neonatal conjunctivitis.
What Are the Symptoms of Conjunctivitis?
The most common symptoms of pink eye include redness, discharge, and irritation. The specific type of discharge—watery, thick, or stringy—helps distinguish between viral, bacterial, and allergic conjunctivitis.
- Red or pink appearance
- Eye irritation or discomfort
- Tearing
- Discharge (varies by type)
- Swelling of conjunctiva or eyelids
How Is Conjunctivitis Diagnosed?
Conjunctivitis is usually diagnosed through a clinical examination based on your symptoms, the type of discharge, and your medical history. Most cases do not require laboratory testing, but cultures may be taken for severe or atypical presentations.
Clinical Examination
- Assessment of discharge type
- Evaluation of conjunctiva
- Check for lymph node swelling
- Vision testing
- Slit-lamp examination if needed
When Testing May Be Done
- Severe or atypical cases
- Not responding to treatment
- Suspected gonococcal or chlamydial infection
- Neonatal conjunctivitis
How Is Conjunctivitis Treated?
Treatment depends on the type of conjunctivitis. Most cases can be managed with cool compresses, artificial tears, and good hygiene. Bacterial forms may need antibiotic drops, while allergic conjunctivitis responds to antihistamine drops and allergen avoidance.
Artificial tears help keep the eye lubricated, and careful hand hygiene prevents spread. For evidence-based home care strategies, see our guide on pink eye home remedies. Serious types like gonococcal or neonatal conjunctivitis need prompt, specialized treatment. Contact lens wearers should stop wearing lenses until the condition fully resolves.
If symptoms do not improve within a week, or if you experience significant pain or vision changes, see an eye doctor for evaluation.
For detailed treatment information, see the pages for viral, bacterial, allergic, gonococcal, chlamydial, and neonatal conjunctivitis.
How Can You Prevent Conjunctivitis?
The best ways to prevent conjunctivitis are frequent handwashing, avoiding touching your eyes, and not sharing personal items like towels or eye makeup. During an active infection, strict hygiene prevents spreading it to others.
- Wash hands frequently and avoid touching or rubbing your eyes
- Don't share towels, pillows, or eye makeup
- Change pillowcases daily during an active infection
- Discard eye makeup used while infected
- Stay home while contagious (viral: 10–14 days; bacterial: 24–48 hours after starting antibiotics)
- Contact lens wearers should stop lens use during infection and discard affected lenses and cases
For details on contagiousness and return-to-work/school guidelines, see our guide on is pink eye contagious?. For information on how long pink eye lasts by type, see our duration guide. Parents can find school policies and child-specific advice in our guide on pink eye in children.
For comprehensive prevention and hygiene guidance—especially around infectious spread—see viral conjunctivitis.
When Should You See a Doctor for Conjunctivitis?
Most mild cases of pink eye improve on their own within a week, but certain symptoms require prompt medical evaluation. See a doctor if you experience significant pain, vision changes, or symptoms that are not improving. Keep in mind that not every red eye is pink eye — several other conditions can look similar. See our guide on conditions mistaken for pink eye.
See an eye doctor if you experience:
- Significant eye pain (not just irritation)
- Vision changes or blurring
- Sensitivity to light
- Symptoms not improving after a week
- Severe discharge
- Recent eye surgery or contact lens wear complications
- Immunocompromised status
Seek immediate care for:
- Newborn with eye discharge (within first month of life)
- Suspected chemical exposure
- Severe pain or vision loss
- Contact lens wearer with pain—could be serious infection
Frequently Asked Questions
How can I tell if it's viral or bacterial?
Viral: watery discharge, one eye first, often with cold symptoms, may have swollen lymph node by ear. Bacterial: thick yellow-green discharge, lids stuck shut in morning. However, distinguishing can be difficult, and some cases need professional evaluation.
Do I need antibiotics?
Viral conjunctivitis doesn't respond to antibiotics—it needs to run its course. Bacterial conjunctivitis may resolve on its own, but antibiotics can speed recovery and reduce contagiousness. Allergic conjunctivitis needs allergy treatment, not antibiotics.
How long am I contagious?
Viral: typically 10-14 days from symptom onset. Bacterial: until 24-48 hours after starting antibiotic drops, or about 5-7 days if untreated. Allergic conjunctivitis is not contagious.
Can I go to work or school?
With viral or bacterial conjunctivitis, it's best to stay home while symptomatic and contagious. Children should stay home from school. Allergic conjunctivitis is not contagious, so isolation isn't needed.
Should I throw away my makeup?
Yes, discard any eye makeup (mascara, eyeliner) used during the infection, as it can harbor bacteria or viruses and cause reinfection.
Why do I keep getting conjunctivitis?
Recurrent conjunctivitis may be due to allergies (seasonal patterns), underlying eyelid conditions (blepharitis), chronic dry eye, or environmental factors. See an eye doctor if conjunctivitis keeps returning. For a detailed look at causes and solutions, see our guide on recurring pink eye.
References
Medical Disclaimer: This information is for educational purposes only and does not replace professional medical advice, diagnosis, or treatment. If you have concerns about conjunctivitis or any eye symptoms, please consult a qualified healthcare provider.
Sources:
- American Academy of Ophthalmology. Conjunctivitis.
- Centers for Disease Control and Prevention. Conjunctivitis (Pink Eye).
- Azari AA, Barney NP. Conjunctivitis: a systematic review of diagnosis and treatment. JAMA. 2013;310(16):1721-1729.
- American Academy of Ophthalmology Cornea/External Disease Panel. Conjunctivitis Preferred Practice Pattern. Ophthalmology. 2019.
