Allergic Conjunctivitis
Eye allergies causing itching, redness, and tearing. Learn about seasonal and perennial allergies, treatments, and how to get relief.
Allergic conjunctivitis is inflammation of the conjunctiva (the clear membrane covering the white of the eye and inner eyelids) caused by an allergic reaction. It's extremely common, affecting up to 40% of the population, and while not contagious or sight-threatening, it can significantly impact quality of life.
Key Takeaways
- Itching is the hallmark symptom—distinguishes allergy from infection
- Not contagious—safe to be around others
- Two main types: seasonal (pollen) and perennial (year-round allergens)
- Treatments include antihistamine drops, mast cell stabilizers, and avoiding triggers
- Cool compresses provide immediate relief
- Does not cause permanent vision damage
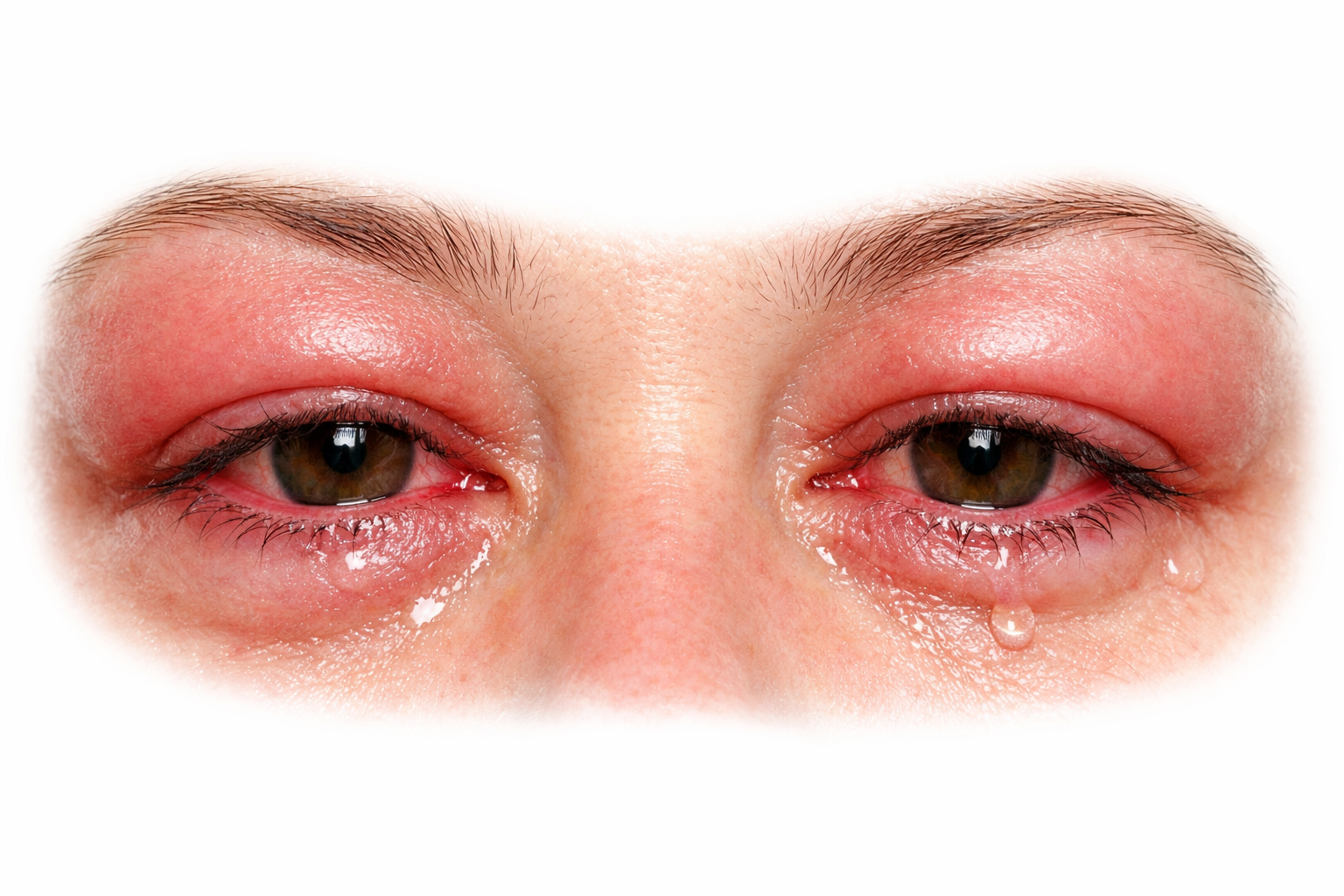
What Are the Symptoms of Allergic Conjunctivitis?
The hallmark symptom of allergic conjunctivitis is intense itching—this is what most clearly distinguishes it from viral or bacterial pink eye. Both eyes are usually affected equally, often alongside other allergy symptoms like sneezing and nasal congestion.
Classic Presentation
- Intense itching—the most characteristic symptom
- Redness (both eyes typically)
- Watery discharge (clear, not thick)
- Eyelid swelling
- Burning sensation
- Gritty feeling
- Light sensitivity
- Puffy eyelids
What Makes It Worse
- Rubbing eyes (provides temporary relief but worsens symptoms)
- Exposure to allergens
- Wind
- Dust
Associated Symptoms
- Sneezing
- Runny nose
- Nasal congestion
- Itchy throat
- General allergic symptoms
What Are the Types of Allergic Conjunctivitis?
There are five main types of allergic conjunctivitis, ranging from mild seasonal allergies to severe forms that can affect the cornea. Seasonal and perennial are by far the most common and are usually manageable with over-the-counter treatments.
Seasonal Allergic Conjunctivitis (SAC)
- Most common type
- Occurs during specific seasons
- Triggered by outdoor allergens:
- Tree pollen (spring)
- Grass pollen (late spring/summer)
- Ragweed pollen (fall)
Perennial Allergic Conjunctivitis (PAC)
- Year-round symptoms
- Triggered by indoor allergens:
- Dust mites
- Pet dander
- Mold
- Cockroaches
Vernal Keratoconjunctivitis (VKC)
- More severe form
- Usually in children/young adults — see our guide on pink eye in children
- Worse in spring and summer
- Large papillae under upper lid
- Can affect cornea
- Requires specialist care
Atopic Keratoconjunctivitis (AKC)
- Associated with atopic dermatitis (eczema)
- Year-round symptoms
- More serious, can cause corneal scarring
- Requires ongoing management
Giant Papillary Conjunctivitis (GPC)
- Related to contact lens wear or foreign bodies
- Large bumps under upper lid
- Often requires discontinuing lenses
- See giant papillary conjunctivitis
How Is Allergic Conjunctivitis Diagnosed?
Allergic conjunctivitis is usually diagnosed clinically based on your symptoms, allergy history, and the seasonal pattern of your symptoms. The presence of intense itching with bilateral involvement in someone with known allergies is highly suggestive.
Usually clinical based on:
- Characteristic symptoms (itching!)
- Both eyes affected
- Allergic history
- Seasonal pattern
Eye Examination
- Conjunctival redness
- Watery discharge
- Lid swelling
- May see papillae (tiny bumps) on conjunctiva
When Further Testing Needed
- Allergy skin testing or blood tests (to identify specific allergens)
- Conjunctival scraping (rarely needed)
How Is Allergic Conjunctivitis Treated?
Treatment focuses on three strategies: avoiding allergen triggers, using medications to control symptoms, and providing immediate relief with cool compresses and artificial tears. Most mild to moderate cases respond well to over-the-counter antihistamine eye drops.
Immediate Relief
Quick relief measures:
- Cool compresses—apply to closed eyes for 10-15 minutes
- Artificial tears—wash away allergens, soothe irritation
- Stop rubbing—rubbing releases more histamine and worsens symptoms
- Refrigerate eye drops—cold drops feel more soothing
- For more home care tips, see our pink eye home remedies guide
Avoidance
- Stay indoors when pollen counts are high
- Keep windows closed during allergy season
- Shower and change clothes after outdoor activities
- Use air conditioning with HEPA filter
- Wash bedding frequently in hot water
- Remove pets from bedroom if allergic
- Use allergen-proof pillow covers
Over-the-Counter Medications
Artificial Tears
- Dilute and wash out allergens
- Soothe irritated eyes
- Safe for frequent use
Antihistamine/Mast Cell Stabilizer Drops
- Ketotifen (Zaditor, Alaway)—very effective OTC option
- Work quickly and prevent symptoms
- Use once or twice daily
- Good for seasonal allergies
Oral Antihistamines
- Help with overall allergic symptoms
- May cause dry eyes as side effect
- Newer generation (loratadine, cetirizine) less sedating
Prescription Medications
Stronger Antihistamine/Mast Cell Stabilizers
- Olopatadine (Patanol, Pataday)
- Alcaftadine (Lastacaft)
- Bepotastine (Bepreve)
- Usually dosed once daily
Topical NSAIDs
- Ketorolac
- Reduce inflammation
- Useful for itching
Topical Corticosteroids
- Loteprednol (Lotemax)—preferred for allergic conjunctivitis due to lower risk of IOP elevation
- Reserved for severe cases
- Effective but have risks with long-term use
- Requires monitoring
- Used for short courses
Mast Cell Stabilizers Only
- Cromolyn sodium
- Better for prevention than acute treatment
- Need to start before allergy season
Immunotherapy
For severe, persistent allergic conjunctivitis:
- Allergy shots (subcutaneous immunotherapy)
- Sublingual tablets (for some allergens)
- Desensitizes immune system over time
- Requires allergist evaluation
Contact Lens Wearers
If you have eye allergies and wear contact lenses:
- Consider daily disposable lenses (fresh lens each day)
- Don't wear lenses when symptoms are severe
- Use preservative-free drops compatible with contacts
- Remove lenses before using medicated drops (unless approved for use with contacts)
- May need to reduce wear time during allergy season
How Can You Tell Allergic Conjunctivitis from Viral Pink Eye?
The key difference is itching: allergic conjunctivitis causes intense itching, while viral pink eye causes mild or no itch. Allergic conjunctivitis affects both eyes equally and is not contagious, while viral pink eye often starts in one eye and is highly contagious. For a detailed comparison, see our guide on pink eye vs allergies and bacterial vs viral vs allergic pink eye.
| Feature | Allergic | Viral |
|---|---|---|
| Itching | Prominent | Mild or absent |
| Discharge | Watery | Watery |
| Contagious | No | Yes |
| Pattern | Both eyes equally | Often starts one eye |
| Systemic symptoms | Allergies (sneezing, etc.) | Cold symptoms possible |
| Duration | While exposed to allergen | 1-3 weeks then resolves |
When Should You See a Doctor for Allergic Conjunctivitis?
See a doctor if over-the-counter treatments aren't providing relief, or if you develop symptoms that suggest something other than allergies—such as thick colored discharge, significant pain, or vision changes. One-sided symptoms or severe light sensitivity also warrant evaluation.
See a doctor if:
- Symptoms don't improve with OTC treatment
- Significant eye pain
- Vision changes
- Thick or colored discharge (may indicate infection)
- Symptoms in only one eye
- Sensitivity to light is severe
- Contact lens wearer with symptoms
What Are the Complications of Allergic Conjunctivitis?
Simple allergic conjunctivitis (seasonal and perennial) is not sight-threatening and does not cause permanent damage. However, severe forms like vernal and atopic keratoconjunctivitis can affect the cornea and require specialist management.
Usually Mild
- Allergic shiners (dark circles under eyes)
- Lid swelling
- Temporary blurry vision from tearing
Potential (With Severe Forms)
- Corneal involvement (VKC, AKC)
- Corneal ulcers (rare)
- Steroid side effects from prolonged use
How Can You Prevent Allergic Conjunctivitis?
While you can't prevent the underlying allergy, you can significantly reduce symptoms through environmental control and starting preventive medications before allergy season begins. Wearing sunglasses outdoors reduces allergen contact with the eyes.
Environmental Control
- Check pollen counts and limit outdoor time when high
- Wear sunglasses outdoors (reduces allergen contact)
- Don't rub eyes
- Remove makeup thoroughly
- Keep pets out of bedroom
- Use high-efficiency air filters
Prophylactic Medication
- Start antihistamine/mast cell stabilizer drops before allergy season
- Continue daily during season
- More effective preventing symptoms than treating them
- If symptoms keep returning despite prevention, see our guide on recurring pink eye
Frequently Asked Questions
Why do my eyes itch so much?
Itching occurs when allergens trigger mast cells in the conjunctiva to release histamine and other chemicals. These substances cause the intense itching sensation that's characteristic of allergic conjunctivitis.
Can eye allergies cause permanent damage?
Simple allergic conjunctivitis (SAC and PAC) does not cause permanent damage. However, severe forms like VKC and AKC can potentially affect the cornea. These require proper management.
Are eye allergies contagious?
No. Allergic conjunctivitis is an immune response to allergens, not an infection. You cannot spread it to others.
Can I prevent eye allergies?
You can reduce symptoms by avoiding triggers, but you can't prevent the underlying allergic tendency. Starting preventive medications before your allergy season can significantly reduce symptoms.
Why do my eyes swell so much?
The loose tissue around the eyes (conjunctiva and eyelids) swells easily when histamine is released. This puffiness usually resolves when the allergic exposure ends and treatment is used.
Can I wear contacts during allergy season?
Many people can, with modifications. Daily disposables are best. You may need to reduce wear time or use glasses on high-pollen days. Some people switch to glasses during peak season.
References
Medical Disclaimer: This information is for educational purposes only and does not replace professional medical advice, diagnosis, or treatment. If you have eye symptoms, please consult a qualified healthcare provider.
Sources:
- American Academy of Ophthalmology. Allergic Conjunctivitis.
- American College of Allergy, Asthma & Immunology. Eye Allergy.
- Bielory L, et al. Allergic conjunctivitis: Update on pathophysiology and prospects for future treatment. J Allergy Clin Immunol. 2020;145(5):1275-1291.
