Bacterial Conjunctivitis
A common eye infection causing red eyes with mucopurulent discharge. Learn about causes, symptoms, treatment, and when antibiotics are needed.
Bacterial conjunctivitis is an infection of the conjunctiva (the clear membrane covering the white of the eye and inner eyelids) caused by bacteria. It's one of the most common eye infections, characterized by red eyes with thick, purulent (pus-like) discharge. While usually self-limiting, antibiotic treatment speeds recovery and reduces contagion.
Key Takeaways
- Common bacterial eye infection affecting all ages
- Hallmark sign: thick, yellow-green discharge that accumulates overnight
- Usually self-limiting but antibiotics speed recovery
- Highly contagious—good hygiene essential
- Usually resolves in 5-7 days with treatment
- See a doctor for severe cases, contact lens wearers, or if vision affected
What Causes Bacterial Conjunctivitis?
Bacterial conjunctivitis is most commonly caused by Staphylococcus aureus in adults and Haemophilus influenzae in children. The infection spreads through direct contact with infected secretions, contaminated hands, or shared personal items like towels and eye makeup.
Common Bacteria
In Adults:
- Staphylococcus aureus—most common
- Staphylococcus epidermidis
- Streptococcus pneumoniae
- Haemophilus influenzae
- Moraxella catarrhalis
In Children:
- Haemophilus influenzae—most common
- Streptococcus pneumoniae
- Moraxella catarrhalis
Less Common but More Serious
- Pseudomonas aeruginosa—especially in contact lens wearers
- Neisseria gonorrhoeae—gonococcal conjunctivitis
- Chlamydia trachomatis—chlamydial conjunctivitis
How It Spreads
- Direct contact with infected secretions
- Contaminated hands touching eyes
- Sharing towels, pillows, or eye makeup
- Contaminated contact lenses or solutions
- Spread from infected sinuses or ears
What Are the Symptoms of Bacterial Pink Eye?
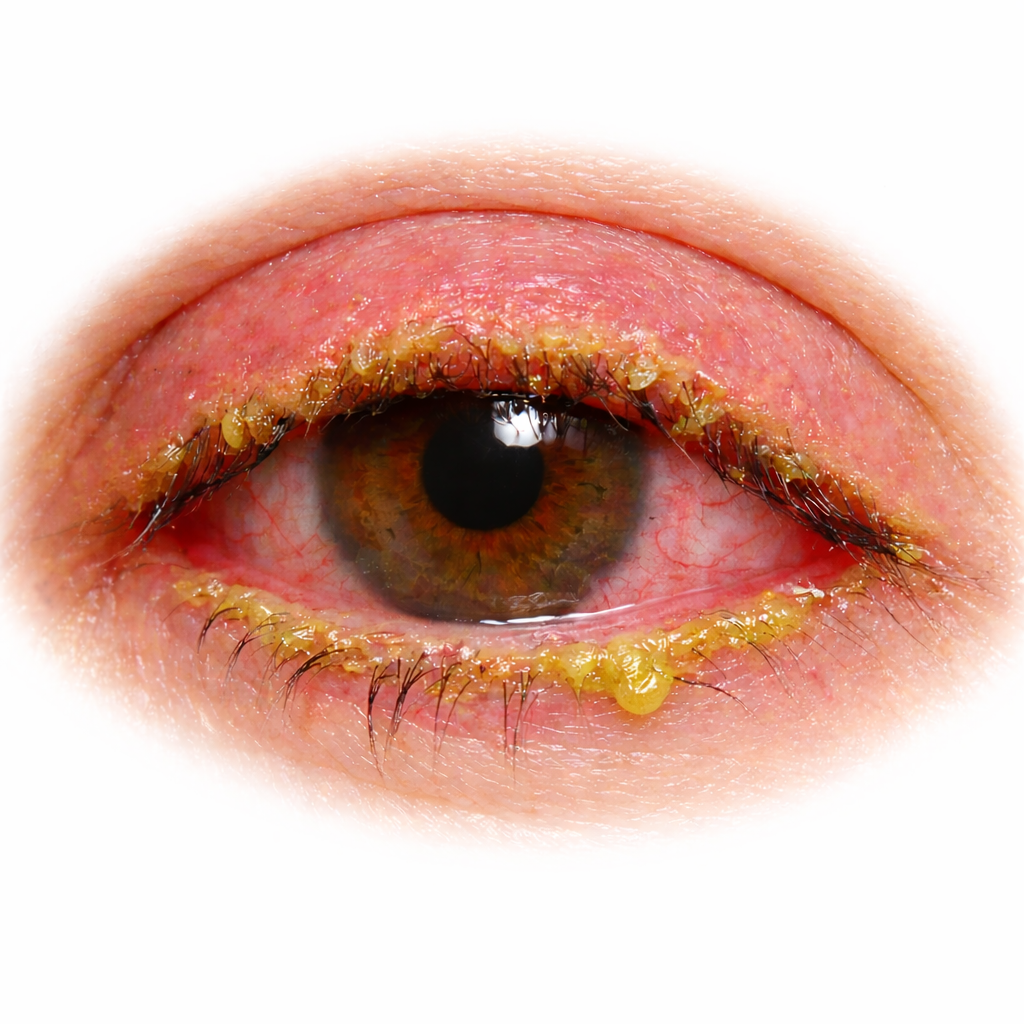
The hallmark of bacterial conjunctivitis is thick, yellow-green discharge that accumulates overnight and often "glues" the eyelids shut by morning. Eyes are red and irritated, with a foreign body sensation and mild to moderate discomfort rather than severe pain.
Classic Presentation
- Red, irritated eyes (one or both)
- Thick discharge—yellow, green, or white
- Crusting of lids—especially upon waking ("eyes stuck shut")
- Foreign body sensation
- Mild to moderate discomfort (not severe pain)
- Tearing
- Lid swelling
What Distinguishes Bacterial from Viral
For a full comparison of all three main types, see our guide on bacterial vs viral vs allergic pink eye.
| Feature | Bacterial | Viral |
|---|---|---|
| Discharge | Thick, purulent | Watery |
| Crusting | Heavy | Minimal |
| Eye involvement | Often one eye first, then second | Often both eyes |
| Associated symptoms | Usually isolated | May have cold symptoms |
| Preauricular node | Usually absent | Often present |
Timeline
- Onset: Often rapid (overnight)
- Without treatment: May resolve in 7-10 days
- With treatment: Usually improves within 24-48 hours
How Is Bacterial Conjunctivitis Diagnosed?
Bacterial conjunctivitis is usually diagnosed through a clinical examination, evaluating the type of discharge, lid appearance, and whether vision is affected. Lab cultures are not routine but may be ordered for severe, non-responsive, or high-risk cases.
Clinical Examination
- History and symptom review
- Examination of discharge character
- Evaluation of lid and conjunctival appearance
- Check for corneal involvement
- Assessment of vision
When Cultures Are Needed
Bacterial cultures are not routine but considered for:
- Severe or hyperacute cases
- Neonatal conjunctivitis
- Cases not responding to initial treatment
- Suspected gonococcal or chlamydial infection
- Contact lens-related infections
- Immunocompromised patients
How Is Bacterial Pink Eye Treated?
Most bacterial conjunctivitis is treated with antibiotic eye drops or ointment, which speeds recovery and reduces contagiousness. Mild cases may resolve on their own in 7–10 days, but treatment typically clears the infection within 2–5 days.
Antibiotic Eye Drops
First-line treatment for most cases:
Commonly Prescribed:
- Erythromycin ointment (especially for children)
- Polymyxin B/trimethoprim drops
- Fluoroquinolones (ofloxacin, moxifloxacin, ciprofloxacin)
- Azithromycin drops
- Tobradex (tobramycin/dexamethasone)—when bacterial infection has steroid-responsive inflammation
Typical Regimen:
- Drops: 4 times daily for 5-7 days
- Ointment: 2-3 times daily for 5-7 days
- Continue for full course even if improving
Supportive Care
- Warm compresses to remove crusts
- Gentle lid hygiene
- Artificial tears for comfort
- Cool compresses for swelling
- For more home care tips, see our pink eye home remedies guide
When Not to Use Over-the-Counter Drops
See a doctor rather than self-treating if:
- Contact lens wearer
- Vision is affected
- Significant pain (not just irritation)
- Symptoms not improving after 2-3 days
- Light sensitivity
- Recent eye surgery
- Only one eye affected with severe symptoms
- History of herpes eye infection
Is Bacterial Pink Eye Contagious?
Yes—bacterial conjunctivitis is contagious through direct contact with infected eye secretions, contaminated hands, or shared personal items. Contagiousness decreases significantly within 24–48 hours of starting antibiotic treatment. Without treatment, it remains contagious for up to 5–7 days. For a full breakdown of contagiousness by type, see our guide on is pink eye contagious?.
- With antibiotics: Contagious for approximately 24–48 hours after starting treatment
- Without antibiotics: Contagious for 5–7 days or until discharge resolves
- Return to work/school: Generally safe 24 hours after starting antibiotics and when discharge has improved
- Prevent spread: Wash hands frequently, don't share personal items, and avoid touching your eyes
How Long Does Bacterial Pink Eye Last?
With antibiotic treatment, bacterial conjunctivitis typically improves within 24–48 hours and resolves fully in about 5–7 days. Without treatment, mild cases may self-resolve in 7–10 days, though some can persist or worsen. For a comparison of duration across all types, see our guide on how long pink eye lasts.
- With antibiotic treatment: Noticeable improvement in 1–2 days, full resolution in 5–7 days
- Without treatment: May resolve in 7–10 days, but risk of complications is higher
- Onset: Often rapid—symptoms may appear overnight
- Complete the full course: Continue antibiotic drops for the prescribed duration even if symptoms improve
Special Situations
Contact Lens Wearers
Contact lens-related bacterial conjunctivitis is more concerning:
- Higher risk of Pseudomonas infection
- Can progress to corneal ulcer
- Must stop wearing contacts immediately
- Requires prompt evaluation
- May need fluoroquinolone drops
- Dispose of current lenses and case
Children and School
- Children are commonly affected
- School/daycare policies vary
- Generally can return 24 hours after starting antibiotics
- Emphasize hand hygiene
- Avoid sharing personal items
- For detailed guidance, see our guide on pink eye in children
Neonatal Conjunctivitis
Newborn eye discharge is a medical emergency.
Neonatal conjunctivitis (ophthalmia neonatorum) can be caused by serious bacteria including gonorrhea and chlamydia. All newborns with eye discharge need urgent medical evaluation.
How Can You Prevent Bacterial Conjunctivitis?
Good hygiene is the most effective way to prevent bacterial conjunctivitis. Wash your hands frequently, avoid touching your eyes, and never share personal items like towels, pillowcases, or eye makeup—especially during an active infection.
During Active Infection
- Wash hands frequently and thoroughly
- Don't touch eyes, then touch other surfaces
- Don't share towels, washcloths, or pillows
- Change pillowcase daily
- Dispose of eye makeup used during infection
- Don't share eye drops
- Stay home from work/school as directed
General Prevention
- Avoid touching eyes with unwashed hands
- Don't share personal eye items
- Replace contact lens cases regularly
- Follow proper contact lens hygiene
- Don't share eye makeup
What Are the Complications of Bacterial Conjunctivitis?
Complications from bacterial conjunctivitis are uncommon but can occur, particularly in contact lens wearers or immunocompromised patients. The most serious risk is spread of infection to the cornea, which can threaten vision.
Rare but Possible
- Corneal involvement (keratitis)
- Spread to other eye
- Chronic or recurrent infection
- Preseptal cellulitis (if severe)
If your symptoms seem unusual or aren't responding to treatment, other conditions may be mimicking bacterial conjunctivitis — see our guide on conditions mistaken for pink eye.
When Should You See a Doctor for Bacterial Pink Eye?
See a doctor if your symptoms don't improve within 2–3 days of starting treatment, or immediately if you have significant pain, vision changes, or are a contact lens wearer. Some warning signs indicate potential complications that need urgent care.
See a doctor if:
- Contact lens wearer with eye redness
- Vision is affected
- Significant pain (not just irritation)
- Symptoms not improving after 2–3 days of treatment
- Light sensitivity
- Recent eye surgery
- Only one eye affected with severe symptoms
Seek immediate care if:
- Vision decreases
- Severe pain develops
- Sensitivity to light
- White spot on cornea
- Eyelid becomes very swollen or red
- Symptoms rapidly worsen
- Fever develops
Frequently Asked Questions
Is bacterial conjunctivitis ("pink eye") always contagious?
Yes, bacterial conjunctivitis is contagious until the discharge resolves. Good hygiene and avoiding sharing personal items helps prevent spread. After 24 hours of antibiotic treatment, contagiousness is significantly reduced.
Do I need antibiotics?
While bacterial conjunctivitis often resolves on its own, antibiotics speed recovery, reduce contagiousness, and decrease the risk of complications. Most eye care providers recommend antibiotic treatment.
How long until I can wear contacts again?
Wait until all symptoms have completely resolved, typically at least 24-48 hours after finishing antibiotic treatment. Use a fresh pair of lenses and a new lens case. Never wear contacts while you have an active eye infection.
Can I use leftover antibiotic drops from before?
No. Using old or expired drops is not recommended. They may be contaminated, expired, or inappropriate for your current infection. See a doctor for a proper prescription.
How did I get this?
Bacteria can be introduced to the eye through contaminated hands, objects, or contact lenses. Sometimes bacteria spread from nearby infections (sinuses, ears). In some cases, the source isn't clear.
Can I go to work or school?
Many workplaces and schools require you to stay home until you've been on antibiotics for 24 hours and discharge has significantly improved. Check your specific policies.
References
Medical Disclaimer: This information is for educational purposes only and does not replace professional medical advice, diagnosis, or treatment. If you have symptoms of eye infection, please consult a qualified healthcare provider.
Sources:
- American Academy of Ophthalmology. Conjunctivitis (Pink Eye).
- Azari AA, Barney NP. Conjunctivitis: a systematic review of diagnosis and treatment. JAMA. 2013;310(16):1721-1729.
- Centers for Disease Control and Prevention. Conjunctivitis (Pink Eye).
