Conditions Mistaken for Pink Eye
Not every red eye is pink eye. Learn about blepharitis, dry eye, keratitis, uveitis, styes, and other conditions commonly confused with conjunctivitis.
A red eye doesn't always mean pink eye. While conjunctivitis is the most common cause of a red eye, many other conditions look similar but require very different treatment. Some of these look-alikes are harmless, while others are sight-threatening emergencies. Knowing the difference can prevent delayed treatment and protect your vision.
Key Takeaways
- Not every red eye is conjunctivitis—several conditions mimic pink eye but need different treatment
- Blepharitis and dry eye are the most common mimics
- Keratitis (corneal infection) and uveitis are serious conditions that can threaten vision
- Pain, light sensitivity, and vision changes suggest something more serious than simple pink eye
- Contact lens wearers with red, painful eyes need urgent evaluation for corneal ulcer
- When in doubt, see an eye doctor—a slit-lamp exam can distinguish these conditions
Not Every Red Eye Is Pink Eye
Pink eye (conjunctivitis) is characterized by redness, discharge, and irritation of the conjunctiva—the clear membrane covering the eye surface. But many other eye conditions cause redness, and some are far more serious. Here's what else could be going on.
Blepharitis
Blepharitis is chronic inflammation of the eyelid margins—the area where your eyelashes grow. It's one of the most common eye conditions and frequently gets mistaken for recurring pink eye.
How it differs from pink eye:
- Redness concentrated at the lid margins rather than across the whole eye
- Flaky, crusty debris at the base of the eyelashes
- Burning and irritation rather than discharge
- Chronic and recurring — doesn't follow an infection timeline
- Often associated with meibomian gland dysfunction
Treatment: Daily lid hygiene, warm compresses, and sometimes antibiotic or anti-inflammatory drops. This is a chronic condition requiring ongoing maintenance, not a one-time treatment.
Dry Eye Syndrome
Dry eye syndrome is a chronic condition where the eyes don't produce enough tears or the tears evaporate too quickly. It can cause persistent redness that's easily confused with conjunctivitis.
How it differs from pink eye:
- Burning, stinging, and gritty sensation rather than discharge
- Symptoms worse with screen use, dry environments, and at the end of the day
- Usually affects both eyes
- No thick discharge — may have some watery tearing as a reflex
- Chronic and persistent rather than acute onset
Treatment: Artificial tears, environmental modifications, lid hygiene, and in some cases prescription drops like cyclosporine. See our guide on why your eyes are dry or irritated.
Keratitis
Keratitis is infection or inflammation of the cornea (the clear front window of the eye). It's more serious than conjunctivitis and can cause permanent scarring and vision loss.
How it differs from pink eye:
- Significant pain — much more than the mild irritation of pink eye
- Light sensitivity — often severe
- Blurred vision — the cornea is directly involved
- May see a white spot on the cornea
- Strongly associated with contact lens wear (especially sleeping in lenses)
Contact lens wearers: a red, painful eye is NOT just pink eye until proven otherwise. Corneal ulcers can look similar to conjunctivitis early on but can scar the cornea permanently. Remove your lens and seek same-day evaluation.
Treatment: Depends on the cause — bacterial keratitis needs aggressive antibiotic drops, fungal keratitis needs antifungal treatment, and herpes simplex keratitis needs antiviral medication. Steroids used for the wrong type of keratitis can be devastating.
Corneal Abrasion
A corneal abrasion is a scratch on the cornea, often from a fingernail, contact lens, or foreign body. It causes sudden-onset redness and pain.
How it differs from pink eye:
- Sudden onset after a specific event (scratch, foreign body, contact lens)
- Significant pain — sharp, stabbing
- Tearing without discharge
- Light sensitivity
- Usually one eye only
Treatment: Antibiotic drops to prevent infection, pain management, and follow-up to ensure healing. Most abrasions heal within 24–48 hours.
Styes and Chalazia
A stye (hordeolum) is an infected bump on the eyelid, while a chalazion is a blocked oil gland that forms a painless lump.
How they differ from pink eye:
- Localized bump on the eyelid rather than diffuse redness
- A stye is tender and red; a chalazion is usually painless
- The eye itself may be mildly red but not the primary feature
- No significant discharge (unless the stye drains)
Treatment: Warm compresses 3–4 times daily for both. Styes may need antibiotic ointment. Persistent chalazia may need in-office drainage.
Uveitis
Uveitis is inflammation of the uvea (the middle layer of the eye including the iris). It's a serious condition that can cause vision loss if untreated.
How it differs from pink eye:
- Deep, aching eye pain — not surface irritation
- Severe light sensitivity — even mild light is uncomfortable
- Blurred vision
- Redness concentrated around the iris (ciliary flush — a ring of redness around the colored part)
- No discharge
- May be associated with autoimmune conditions
Uveitis is a medical urgency. If you have a painful red eye with light sensitivity and blurred vision but no discharge, this may be uveitis—not pink eye. See an ophthalmologist promptly. Delayed treatment can lead to permanent vision loss.
Treatment: Steroid eye drops, dilating drops, and treatment of any underlying systemic cause. Requires ophthalmologist management.
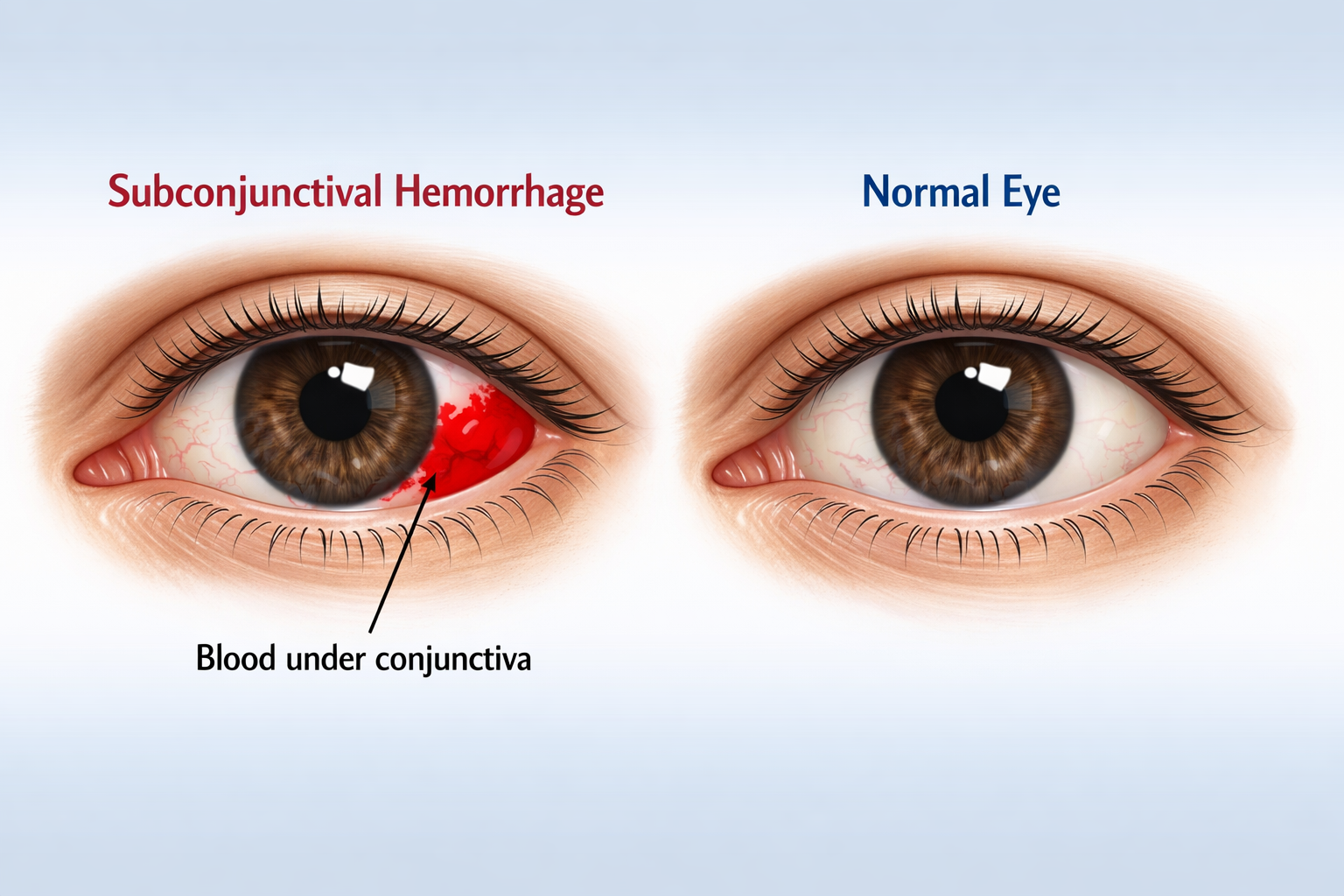
Subconjunctival Hemorrhage
A subconjunctival hemorrhage is a bright red patch on the white of the eye from a broken blood vessel. It looks alarming but is usually harmless.
How it differs from pink eye:
- Bright, blood-red patch — not diffuse pink redness
- No pain, no discharge, no vision change
- Often noticed suddenly (upon looking in a mirror)
- May follow straining, coughing, sneezing, or rubbing
- Resolves on its own in 1–2 weeks
Treatment: No treatment needed. It resolves on its own like a bruise. See a doctor if it happens frequently or you're on blood thinners.
Episcleritis and Scleritis
Episcleritis is mild inflammation of the tissue just under the conjunctiva, while scleritis is deeper and more serious.
Episcleritis:
- Localized patch of redness (often sectoral)
- Mild discomfort
- Usually self-limiting
- Responds to NSAIDs or artificial tears
Scleritis:
- Deep, boring eye pain that may wake you from sleep
- Redness that may appear violaceous (purplish)
- Associated with autoimmune diseases (rheumatoid arthritis, etc.)
- Requires urgent treatment — can cause vision loss
Other Mimics
Several other conditions can be confused with pink eye:
- Pterygium and pinguecula — benign growths on the eye surface that can become irritated and red
- Ocular rosacea — chronic eye redness and irritation associated with facial rosacea
- Chemical eye burns — exposure to irritants or chemicals
- Orbital cellulitis — serious infection of the tissues around the eye causing swelling, redness, pain, and fever (medical emergency)
- Foreign body — something stuck on or in the eye
- Contact lens overwear — chronic redness from excessive lens use
How to Tell the Difference
Use these features to help distinguish pink eye from its mimics:
| Symptom | Likely Pink Eye | Likely Something Else |
|---|---|---|
| Pain level | Mild irritation | Significant pain → keratitis, uveitis, scleritis |
| Discharge | Present (watery or thick) | Absent → uveitis, scleritis, dry eye |
| Light sensitivity | Mild or absent | Severe → keratitis, uveitis |
| Vision | Normal (may blur from discharge) | Decreased → keratitis, uveitis, corneal ulcer |
| Redness pattern | Diffuse across conjunctiva | Ring around iris → uveitis; localized patch → episcleritis |
| Duration | Days to weeks, then resolves | Chronic/recurring → blepharitis, dry eye, rosacea |
When Red Eyes Need Urgent Care
Seek urgent eye care if you have:
- Eye pain that is more than mild irritation
- Vision loss or significant blurring
- Severe photophobia (light sensitivity)
- A white spot on the cornea
- Redness with swelling, warmth, and fever (possible orbital cellulitis)
- Red eye after trauma or chemical exposure
- Red eye in a contact lens wearer with pain
- Symptoms that are progressively worsening despite treatment
A slit-lamp exam by an eye doctor is the definitive way to distinguish these conditions. If you're unsure whether your red eye is simple pink eye or something more serious, it's always better to get checked. See also our guide on do I have an eye infection? and recurring pink eye.
Frequently Asked Questions
How can I tell if my red eye is pink eye or something more serious?
The key warning signs that suggest something other than simple pink eye are: significant pain (not just irritation), vision changes, severe light sensitivity, and the absence of discharge. Pink eye is typically more of a nuisance—irritating but not painful. If your eye hurts, see a doctor.
Can my doctor tell the difference just by looking?
An experienced eye doctor can often distinguish these conditions through clinical examination, especially with a slit-lamp exam. Some cases may need additional testing (cultures, corneal staining, intraocular pressure measurement) to confirm the diagnosis.
I was told I have pink eye but it's not getting better. What else could it be?
If you're not improving after a week of treatment, consider: wrong diagnosis (blepharitis, dry eye, or keratitis instead of conjunctivitis), wrong type (viral treated with antibiotics), chlamydial conjunctivitis (doesn't respond to standard drops), or an underlying condition making you susceptible. Return to your doctor for reevaluation.
Can pink eye turn into something more serious?
Simple conjunctivitis rarely progresses to serious disease. However, untreated bacterial conjunctivitis (especially in contact lens wearers) can spread to the cornea and cause keratitis or corneal ulcer. This is why worsening symptoms warrant reevaluation.
Should I go to the ER for a red eye?
Not for typical pink eye. But go to the ER if you have: severe pain, sudden vision loss, a chemical splash in the eye, red eye with high fever and lid swelling (possible orbital cellulitis), or a penetrating eye injury.
References
Medical Disclaimer: This information is for educational purposes only and does not replace professional medical advice, diagnosis, or treatment. If you have concerns about a red eye, please consult a qualified healthcare provider.
Sources:
- American Academy of Ophthalmology. Conjunctivitis Preferred Practice Pattern.
- Cronau H, Kankanala RR, Mauger T. Diagnosis and management of red eye in primary care. Am Fam Physician. 2010;81(2):137-144.
- Leibowitz HM. The red eye. N Engl J Med. 2000;343(5):345-351.
